Connect With Us
Blog
Blog
Symptoms of Gout
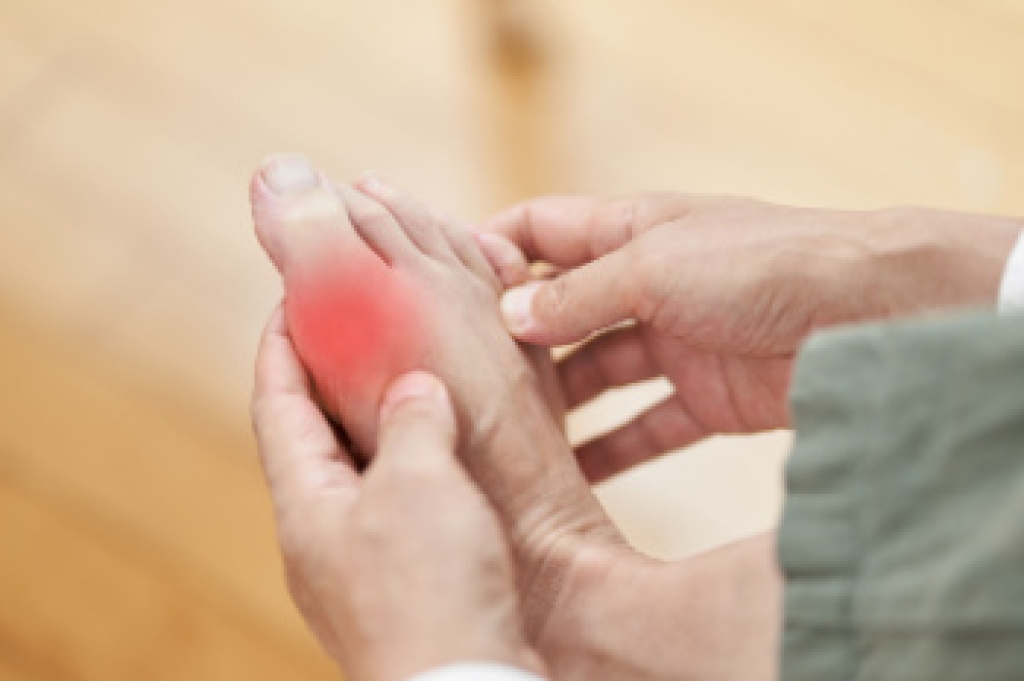
Gout is a form of arthritis that can cause sudden episodes of severe pain in the feet and ankles when uric acid crystals collect inside a joint. Gout frequently affects the big toe, but it may also involve the arch, heel, or ankle. During a flare-up, the joint may become swollen, stiff, and extremely sensitive. Skin often appears red or purple and feels warm to the touch. Some patients describe the pain as sharp, crushing, or pulsating, making it difficult to walk or wear shoes comfortably. Gout attacks may be the result of dehydration, alcohol use, certain medications, or diets high in purine-rich foods. Repeated inflammation can damage cartilage and surrounding tissue. A podiatrist can examine the painful area, evaluate joint changes, and help guide treatment to reduce inflammation and prevent future attacks. Care may include medication recommendations, footwear guidance, and strategies to reduce pressure on the affected joints. If you have symptoms of gout, it is suggested that you schedule an appointment with a podiatrist for relief and prevention tips from this painful condition.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Edward Orman, DPM from Honeygo Podiatry. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our offices located in Perry Hall, and Fallston, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Causes and Symptoms of Heel Pain
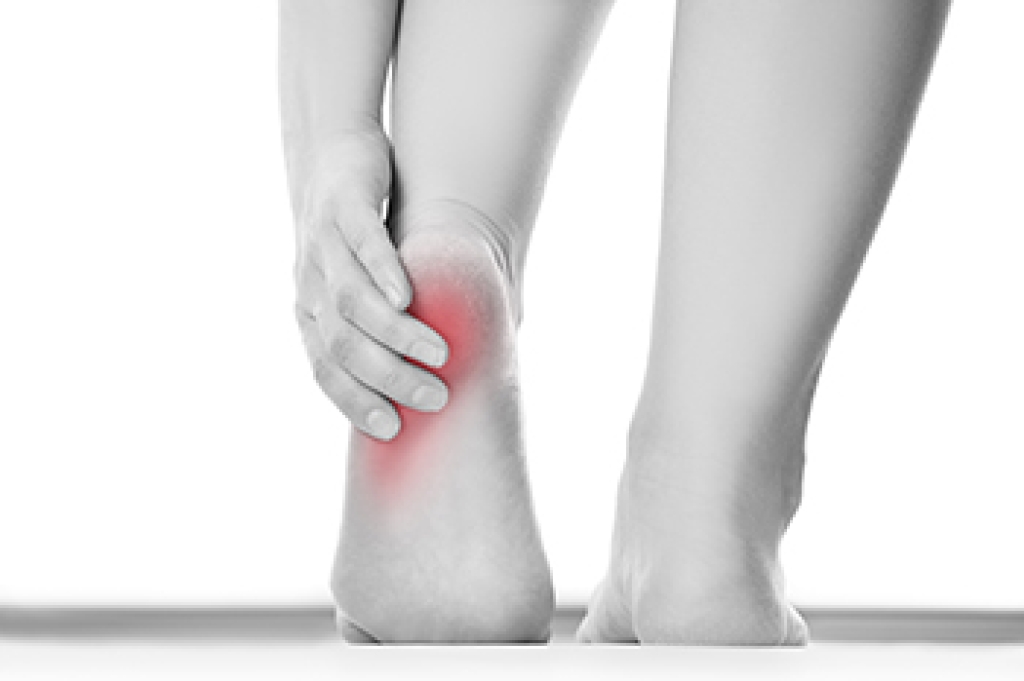
Heel pain is often caused by plantar fasciitis, which is irritation of the thick band of tissue along the bottom of the foot. Another frequent cause of heel pain is Achilles tendonitis, inflammation of the tendon at the back of the heel. Stress fractures from repeated impact, and arthritis, which involves joint wear and stiffness, may also be factors. Nerve irritation, poor circulation, and long periods of standing sometimes play a role. Symptoms include sharp pain with the first steps in the morning and soreness after activity. Swelling or tenderness when pressure is applied to the heel may also occur. Some people notice a dull ache that worsens over time. A podiatrist can evaluate the foot and review symptoms. Imaging may be used to determine the cause. Treatment plans include orthotics, bracing, and guidance to reduce strain and improve foot function. If you have heel pain, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment plan.
Many people suffer from bouts of heel pain. For more information, contact Edward Orman, DPM of Honeygo Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions, please feel free to contact our offices located in Perry Hall, and Fallston, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Clubfoot and Early Care for Healthy Development

Clubfoot is a congenital foot deformity in which the foot is twisted inward and the toes point downward. It may affect one or both feet and is present at birth. This condition is often linked to genetic factors and differences in muscle and tendon development. Symptoms include a visible inward position of the foot, limited range of motion, and stiffness in the affected area. Early care is important to support proper alignment and function as a child grows. A podiatrist can assess the condition, guide treatment options, and monitor progress to improve mobility and comfort. With timely care, many children achieve strong and functional movement. If your child has been born with symptoms of clubfoot, it is strongly suggested that you promptly schedule a visit with a podiatrist to support healthy foot development.
Congenital foot problems require immediate attention to avoid future complications. If you have any concerns, contact Edward Orman, DPM of Honeygo Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Congenital foot problems are deformities affecting the feet, toes, and/or ankles that children are born with. Some of these conditions have a genetic cause while others just happen. Some specific foot ailments that children may be born with include clubfeet, polydactyly/macrodactyly, and cleft foot. There are several other foot anomalies that can occur congenitally. What all of these conditions have in common is that a child may experience difficulty walking or performing everyday activities, as well as trouble finding footwear that fits their foot deformity. Some of these conditions are more serious than others. Consulting with a podiatrist as early as possible will help in properly diagnosing a child’s foot condition while getting the necessary treatment underway.
What are Causes of Congenital Foot Problem?
A congenital foot problem is one that happens to a child at birth. These conditions can be caused by a genetic predisposition, developmental or positional abnormalities during gestation, or with no known cause.
What are Symptoms of Congenital Foot Problems?
Symptoms vary by the congenital condition. Symptoms may consist of the following:
- Clubfoot, where tendons are shortened, bones are shaped differently, and the Achilles tendon is tight, causing the foot to point in and down. It is also possible for the soles of the feet to face each other.
- Polydactyly, which usually consists of a nubbin or small lump of tissue without a bone, a toe that is partially formed but has no joints, or an extra toe.
- Vertical talus, where the talus bone forms in the wrong position causing other bones in the foot to line up improperly, the front of the foot to point up, and the bottom of the foot to stiffen, with no arch, and to curve out.
- Tarsal coalition, when there is an abnormal connection of two or more bones in the foot leading to severe, rigid flatfoot.
- Cleft foot, where there are missing toes, a V-shaped cleft, and other anatomical differences.
- Macrodactyly, when the toes are abnormally large due to overgrowth of the underlying bone or soft tissue.
Treatment and Prevention
While there is nothing one can do to prevent congenital foot problems, raising awareness and receiving neonatal screenings are important. Early detection by taking your child to a podiatrist leads to the best outcome possible.
If you have any questions, please feel free to contact our offices located in Perry Hall, and Fallston, MD . We offer the newest diagnostic and treatment technologies for all your foot care needs.
When Swelling Develops in the Feet and Ankles
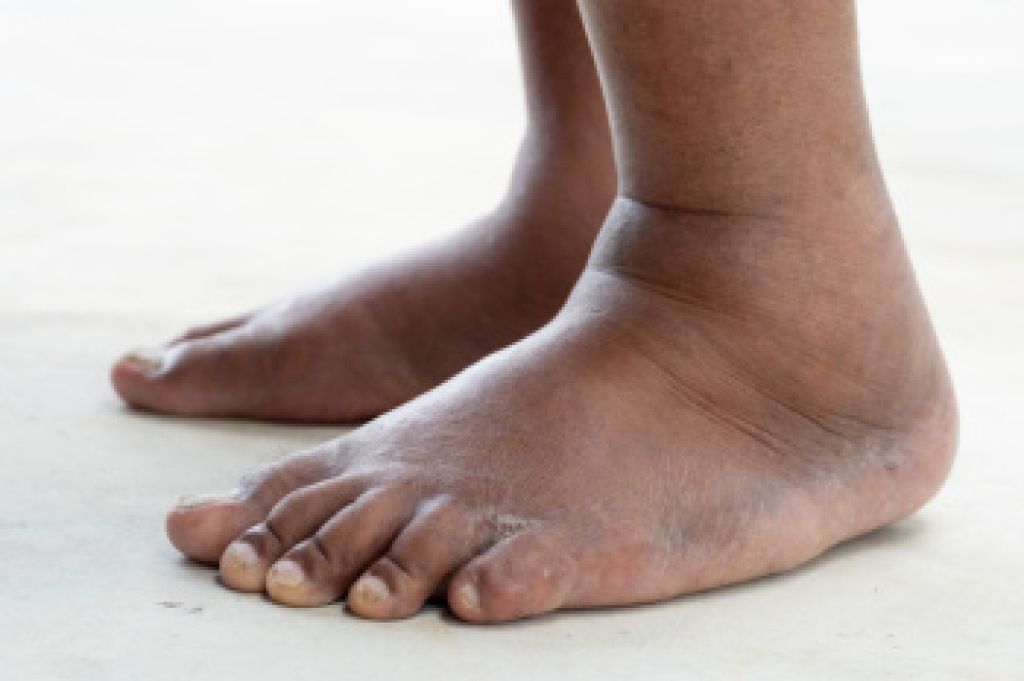
Swollen feet and ankles can occur for several reasons related to fluid balance, circulation, or underlying conditions. This swelling, known as edema, happens when excess fluid collects in the tissues of the lower extremities. These play an important role in supporting body weight and returning blood back toward the heart. Common causes include prolonged standing or sitting, circulation issues, certain medical conditions, and injury that affects normal fluid movement. The swelling may appear gradually or suddenly, causing the skin to look stretched or shiny and feel tight or heavy, and some people notice an indentation after pressing on the area. A podiatrist can evaluate the pattern of swelling through a physical exam and may recommend imaging or coordinate care to identify contributing factors. Treatment includes compression, elevation, wearing supportive footwear, and targeted exercises to improve circulation and reduce fluid buildup. If you have swollen feet and ankles, it is suggested that you schedule an appointment with a podiatrist who can determine what the cause is, and offer effective relief and management solutions.
Swollen feet can be a sign of an underlying condition. If you have any concerns, contact Edward Orman, DPM of Honeygo Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Swollen feet are a common ailment among pregnant women and people who stand or sit for extended periods. Aging may increase the possibility of swollen feet and patients who are obese often notice when their feet are swelling too. There may be medical reasons why swollen feet occur:
- Phlebitis - A condition that causes the veins to become inflamed and can also cause leg pain.
- Liver disease - This may lead to low blood levels of albumin which is a protein. This can cause fluid in the blood to pass into the tissues and several areas of the body can become swollen.
- Heart failure - When the heart doesn’t pump properly the blood that is normally pumped back to the heart can pool in the veins of the legs causing swollen feet.
- Kidney disease - One of the main functions of the kidneys is releasing excess fluid in the body. This type of condition can make it difficult for the kidneys to function properly, and as a result the feet may become swollen.
- Deep-vein thrombosis (DVT)- This is a serious condition where blood clots form in the veins of the legs. They can block the return of blood from the legs to the heart which may cause the feet to swell. It is important to be treated by a podiatrist if this condition is present.
Swollen feet can also be caused by bone and tendon conditions, including fractures, arthritis, and tendinitis. Additionally, there may be skin and toenail conditions and an infection may cause the feet to swell. Patients who take medicine to treat high blood pressure may be prone to getting swollen feet.
Many patients elevate their feet to help relieve the swelling and this is generally a temporary remedy. When a podiatrist is consulted the reason behind the swelling can be uncovered and subsequently treated.
If you have any questions please contact our offices located in Perry Hall, and Fallston, MD . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Blog Archives
- 2026
- 2025
- 2024
- 2023
- 2022